A glioma is a cancer type that involves the glial cell in the brain or spine and accounts for approximately 30% of all brain tumors. Gliomas can be especially aggressive, explaining why they account for 80% of all malignant brain tumors. Since many therapies are initially developed in preclinical animal models, noninvasive approaches facilitate the study of tumor growth and the molecular profile of the tumor. PET and optical imaging are commonly used for molecular imaging, but have the respective drawbacks of requiring the use of radioisotopes or suffering from photon scatter. MSOT has been used to bridge the gap between the limitations of the use of radioactive contrast agents and poor optical spatial resolution to provide noninvasive, high-resolution imaging of the brain with contrast agents that are easily synthesized and handled. It has also been used as a low-cost alternative to BOLD MRI imaging to study the hemodynamics of brain tumors.
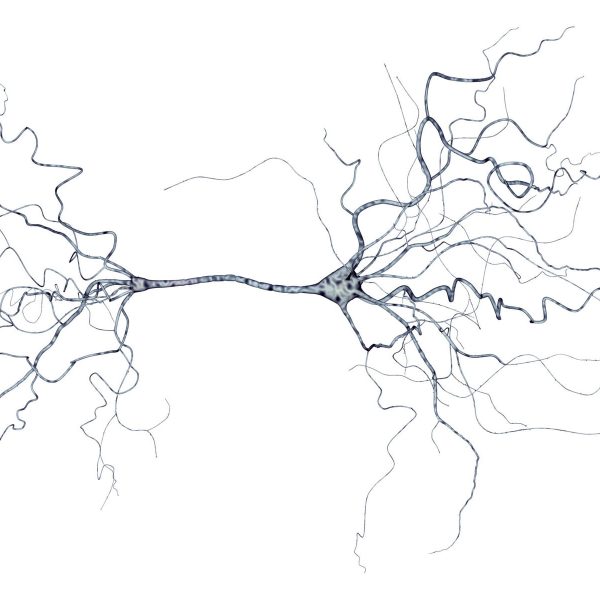
iRFP-containing U87 glioblastoma cells were imaged at multiple positions, which were then rendered in 3D. Single-wavelength MSOT contrast is shown in grayscale, with iRFP signal shown in jet.
Genetic reporters like iRFP absorb light in the near infrared and can be used to label glioblastoma cells. This enables 3D visualization of tumor size and can be used to monitor growth in the brain over time.
Adapted from Deliolanis et al. Mol Imaging Biol. 2014
Noninvasive functional MSOT measurements can track the growth and changes in oxygenation in orthopic glioblastoma.
This approach has also been used to monitor real-time hemodynamic changes and therapeutic efficacy following vascular therapy.
Balasundaram et al. Transl Oncol. 2018
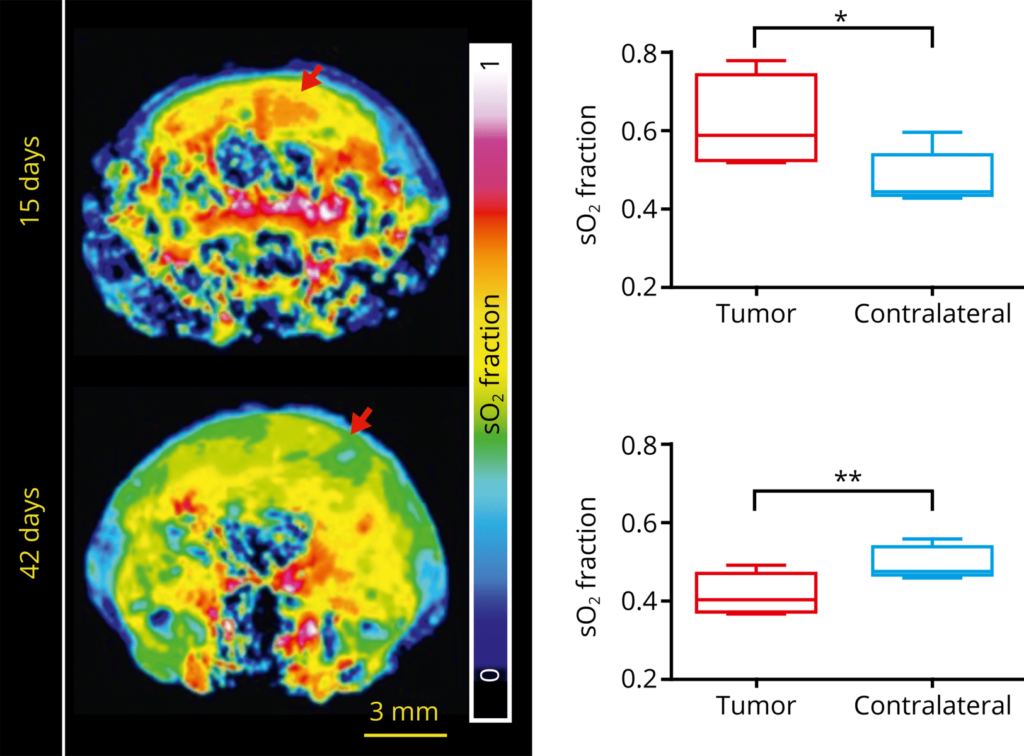
Oxygenation of tumor vs. healthy tissue following vascular disruption
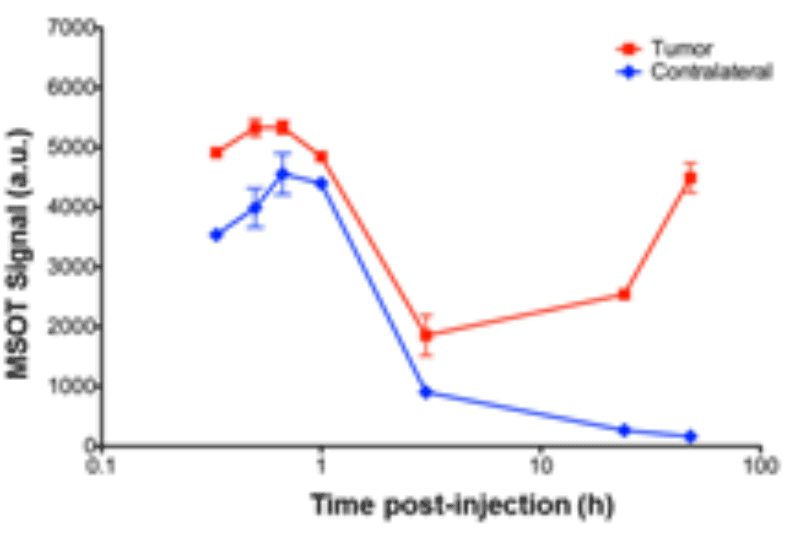
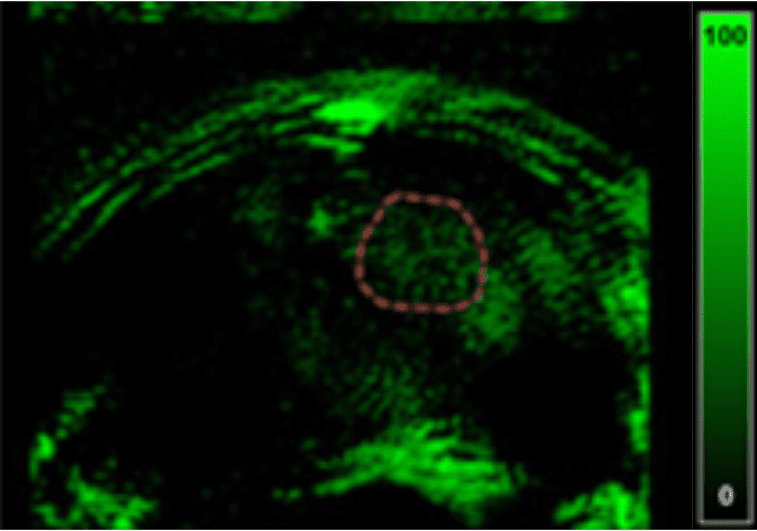
Deoxyglucose measurement in healthy vs. tumor tissue
MSOT enables molecular brain imaging with injected contrast agents, for example by using IRDye800CW-deoxyglucose to image the Warburg effect through the visualization and quantification of glucose metabolism.
Attia et al. J Biophotonics. 2016